What Is Dialysis?
Dialysis is a medical treatment used to replace essential kidney functions when the kidneys are no longer able to adequately filter waste products, excess fluids, and toxins from the blood. By artificially performing these functions, dialysis helps maintain metabolic balance and supports vital organ function.
Dialysis is not a cure for kidney disease; rather, it is a life-sustaining renal replacement therapy for patients with severe or end-stage kidney failure.
Purpose of Dialysis
The primary purposes of dialysis are to:
-
Remove metabolic waste products such as urea and creatinine
-
Eliminate excess fluid from the body
-
Maintain electrolyte balance (sodium, potassium, calcium, phosphate)
-
Help regulate blood pressure
-
Prevent complications related to kidney failure
Through these functions, dialysis plays a critical role in stabilizing patients and improving survival and quality of life.
When Is Dialysis Required?
Dialysis is indicated when kidney function declines to a level where the body can no longer maintain internal balance through conservative medical treatment alone.
Acute Kidney Injury (AKI)
In acute kidney injury, kidney function deteriorates suddenly due to conditions such as severe infection, shock, dehydration, drug toxicity, or trauma. Dialysis may be required temporarily until kidney function recovers.
Chronic Kidney Disease (CKD)
In chronic kidney disease, dialysis is typically initiated when the disease progresses to end-stage renal disease (ESRD), usually when the glomerular filtration rate (GFR) falls below 10–15%.
Common clinical indications include:
-
Persistent fluid overload
-
Severe electrolyte imbalance
-
Uremic symptoms such as nausea, fatigue, or confusion
-
Rising blood urea nitrogen (BUN) and creatinine levels
Main Types of Dialysis
There are three principal dialysis modalities used in modern renal replacement therapy. The selection of an appropriate method depends on clinical condition, hemodynamic stability, lifestyle considerations, and available medical resources.
Hemodialysis (HD)
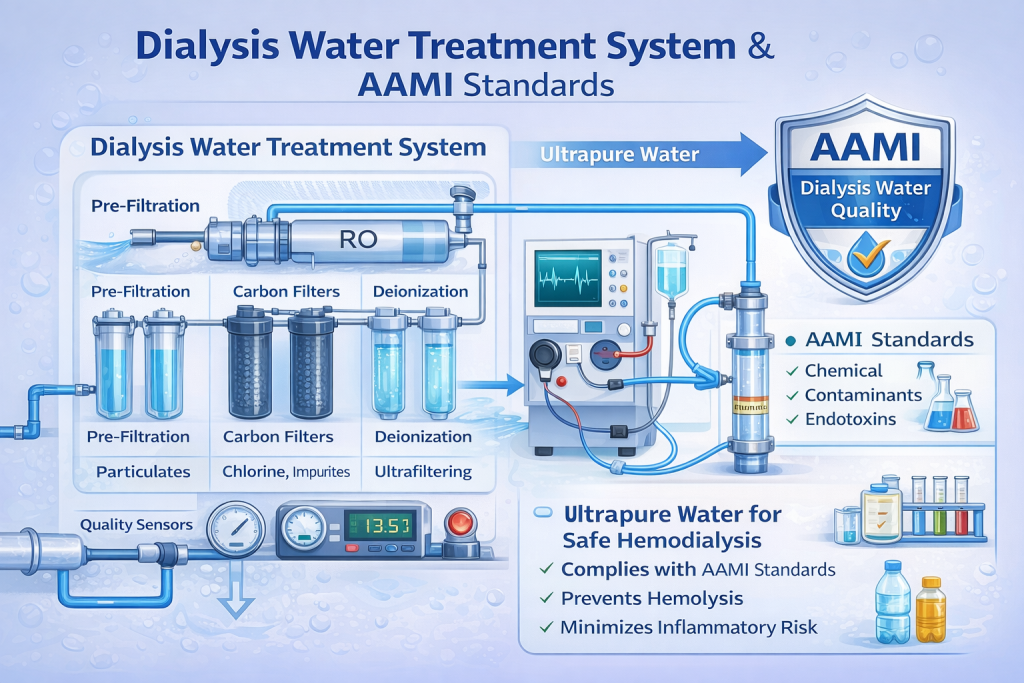
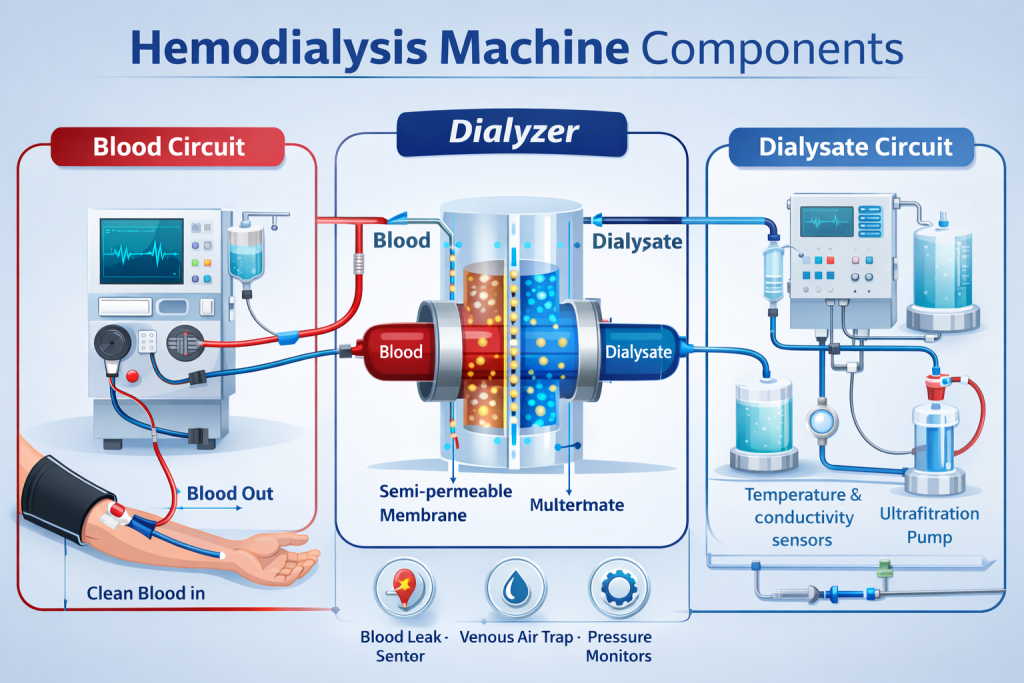
Hemodialysis is the most commonly used dialysis method. Blood is circulated outside the body through a dialysis machine, where it passes through a semi-permeable membrane that removes waste and excess fluid before the blood is returned to the patient.
Key characteristics:
-
Typically performed in dialysis centers or hospitals
-
Commonly scheduled three times per week
-
Each session lasts approximately 3–5 hours
-
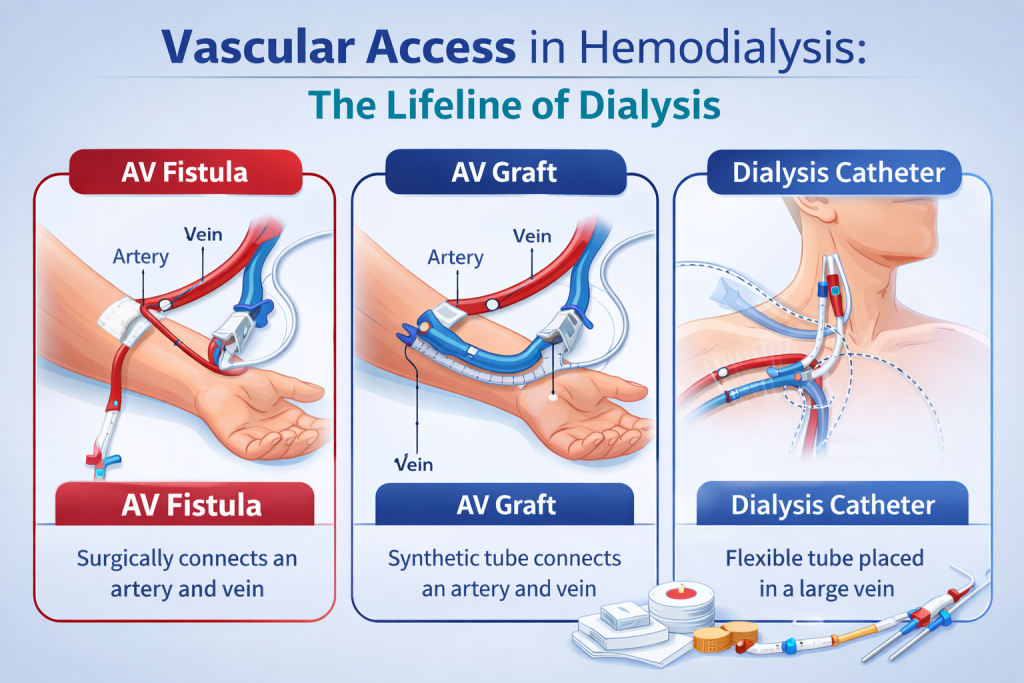
Requires vascular access such as an arteriovenous fistula, graft, or catheter
Advantages:
-
High efficiency in toxin and fluid removal
-
Widely available and clinically established
Limitations:
-
Fixed treatment schedule
-
Potential post-dialysis fatigue or hypotension
Peritoneal Dialysis (PD)
Peritoneal dialysis utilizes the patient’s peritoneal membrane as a natural filtration surface. Dialysis fluid is infused into the abdominal cavity, where waste products diffuse into the fluid and are subsequently drained.
Key characteristics:
-
Can be performed at home
-
Continuous daily therapy
-
Greater flexibility and independence for patients
Advantages:
-
Better preservation of residual kidney function
-
More stable hemodynamic control
Limitations:
-
Risk of peritonitis
-
Requires strict adherence to aseptic technique
Continuous Renal Replacement Therapy (CRRT)
Continuous renal replacement therapy (CRRT) is a slow and continuous dialysis modality primarily used for critically ill patients in intensive care units.
Key characteristics:
-
Continuous operation over 24 hours
-
Suitable for patients with unstable blood pressure
-
Precise control of fluid and electrolyte balance
Advantages:
-
Reduced risk of rapid fluid shifts
-
Improved tolerance in critically ill patients
Limitations:
-
Higher operational cost
-
Requires specialized equipment and trained healthcare professionals
Conclusion
Dialysis is an essential component of renal replacement therapy for patients with advanced kidney failure. A clear understanding of what dialysis is, when it is indicated, and how different modalities such as HD, PD, and CRRT function is crucial for informed clinical decision-making.
Selecting the appropriate dialysis method should be based on medical condition, patient lifestyle, and available healthcare infrastructure to achieve optimal treatment outcomes.