Vascular Access – The Lifeline of Hemodialysis
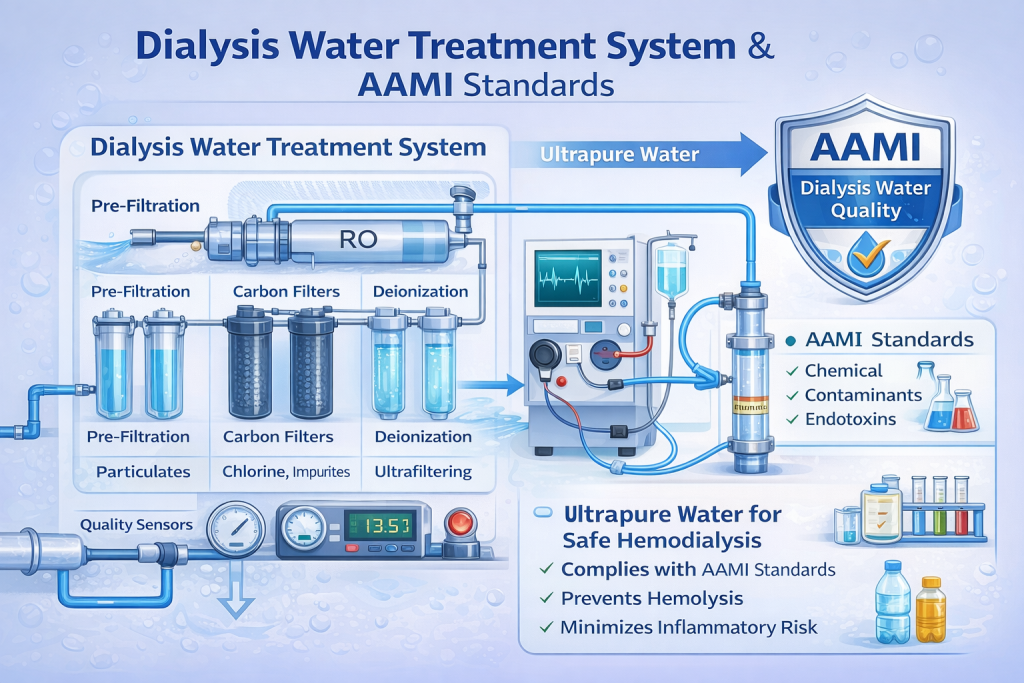
Vascular access is a critical prerequisite for hemodialysis (HD) and is often referred to as the lifeline of dialysis patients. A well-functioning vascular access allows blood to flow efficiently from the patient to the dialysis machine and back, enabling effective removal of toxins and excess fluid.
Proper planning and preparation of vascular access before initiating hemodialysis are essential for long-term treatment success and patient safety.
Importance of Vascular Access Before Hemodialysis
Hemodialysis requires a high blood flow rate, typically close to 1 pint per minute (approximately 450–500 mL/min), to ensure adequate clearance of waste products.
A reliable vascular access must:
-
Provide sufficient blood flow
-
Withstand repeated needle insertions
-
Minimize the risk of infection and thrombosis
-
Support long-term dialysis treatment
Without a suitable vascular access, effective hemodialysis cannot be achieved.
Why Vascular Access Is Required
The primary purpose of vascular access is to:
-
Allow continuous circulation of blood through the dialyzer
-
Maintain stable blood flow and pressure
-
Enable efficient diffusion and convection during dialysis
A properly established access ensures that blood can safely and efficiently pass through the dialysis system multiple times per session.
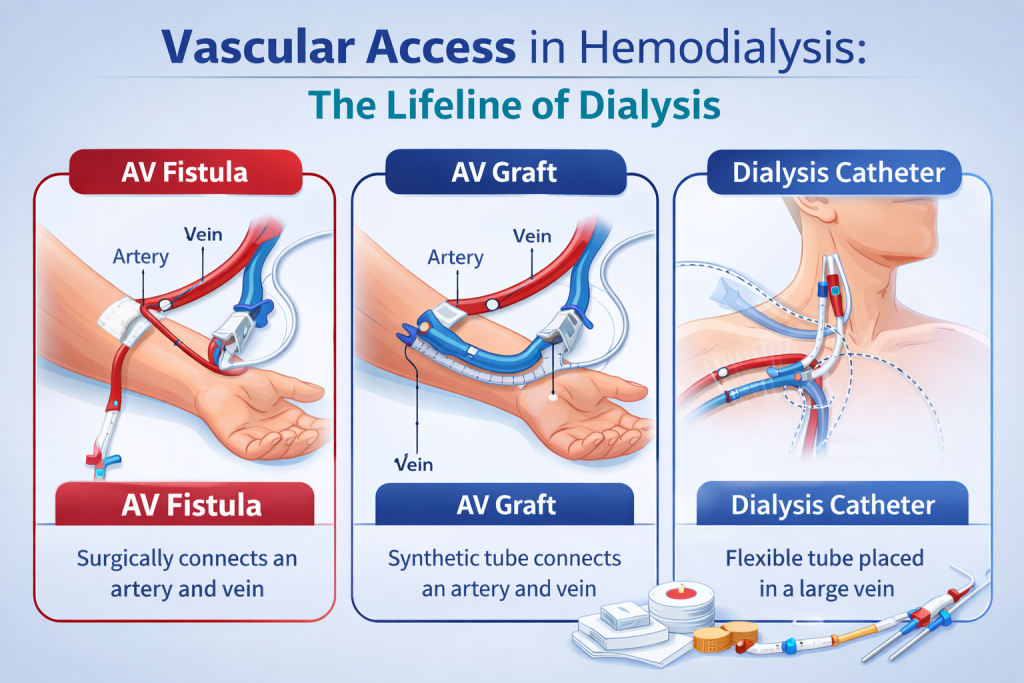
Types of Vascular Access in Hemodialysis
There are three main types of vascular access used in hemodialysis:
1. Arteriovenous Fistula (AV Fistula)
An arteriovenous fistula (AVF) is created surgically by directly connecting an artery to a vein, usually in the forearm or upper arm.
Advantages:
-
Longest lifespan
-
Lowest risk of infection
-
Best blood flow and dialysis efficiency
Limitations:
-
Requires weeks to months to mature
-
Not suitable for all patients due to vascular conditions
AV fistulas are considered the gold standard for long-term hemodialysis access.
2. Arteriovenous Graft (AV Graft)
An AV graft uses a synthetic tube to connect an artery and a vein, serving as an artificial access pathway.
Advantages:
-
Can be used sooner than an AV fistula
-
Suitable for patients with small or weak veins
Limitations:
-
Higher risk of infection and clotting compared to AV fistula
-
Shorter lifespan
AV grafts are an alternative when fistula creation is not feasible.
3. Central Venous Catheter (Dialysis Catheter)
A dialysis catheter is a flexible tube inserted into a large central vein, commonly the internal jugular vein.
Advantages:
-
Immediate use
-
No maturation period required
Limitations:
-
Highest risk of infection
-
Lower blood flow rates
-
Not recommended for long-term use
Catheters are typically used as temporary or emergency access.
Product Relevance and Clinical Supplies
Vascular access preparation and maintenance are closely associated with the following products:
-
Surgical supplies for access creation
-
Dialysis needles and bloodlines
-
Catheters and catheter kits
-
Dressings, bandages, and wound care materials
High-quality consumables play an essential role in preventing complications and maintaining access patency.
Conclusion
Vascular access is the foundation of successful hemodialysis treatment. Understanding the differences between AV fistula, AV graft, and dialysis catheter allows clinicians to select the most appropriate access based on patient condition and treatment goals. Early planning and proper care of vascular access significantly improve dialysis outcomes and patient quality of life.